In addition, screening for comorbidities is, in part, a function of a child’s overweight status. Weight maintenance as they grow in height. This is particularly helpful in the treatment of young children and of those who are merely overweight, in whom the goal may not be weight loss but weight maintenance as they grow in height. 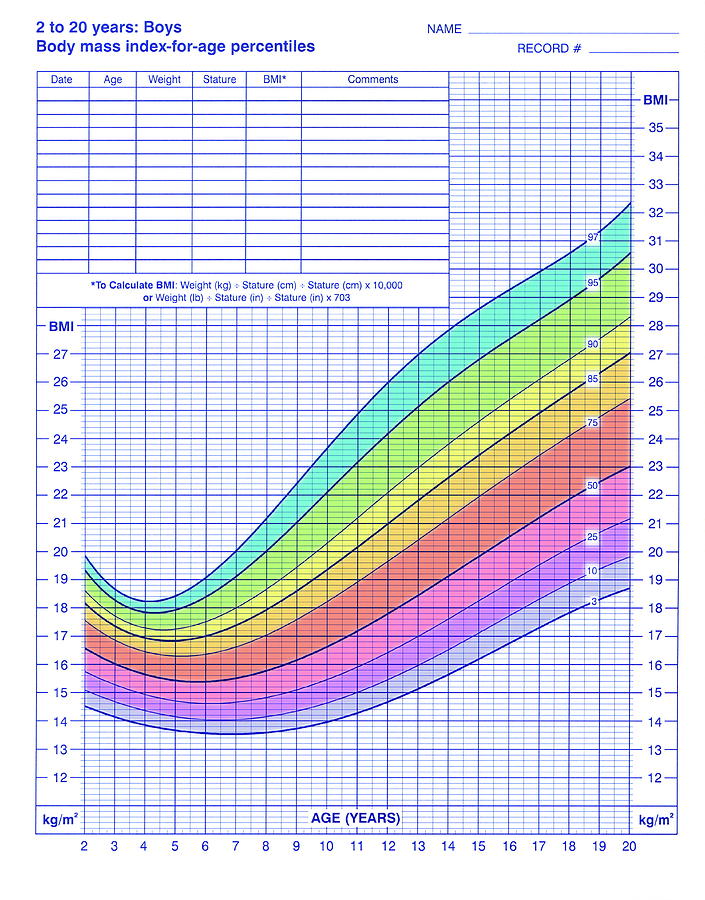
In fact, at least 1 study documents misperception by physicians of about one-third of children.1 Certainly, studies have established that parents have only a limited ability to identify that their child is obese.2-4 Moreover, as you point out, BMI is an excellent tool for tracking results of weight management efforts and can thus serve as both a learning tool and a monitor of progress for child and family alike. I would like to point out that there is no documentation that visual inspection clearly and reliably identifies those children who are obese, especially at mild levels of obesity. You raise the question of whether we should limit use of BMI in children to population studies and simply use inspection as our screening tool, particularly since intervention is relatively unsuccessful. Nonetheless, given that treatment of childhood obesity is so seldom satisfactory, even this use seems of negligible value.- John DiTraglia, MD Portsmouth, Ohio 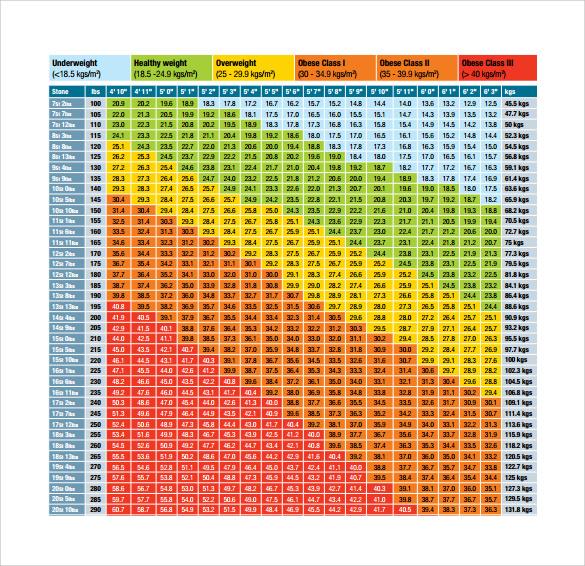
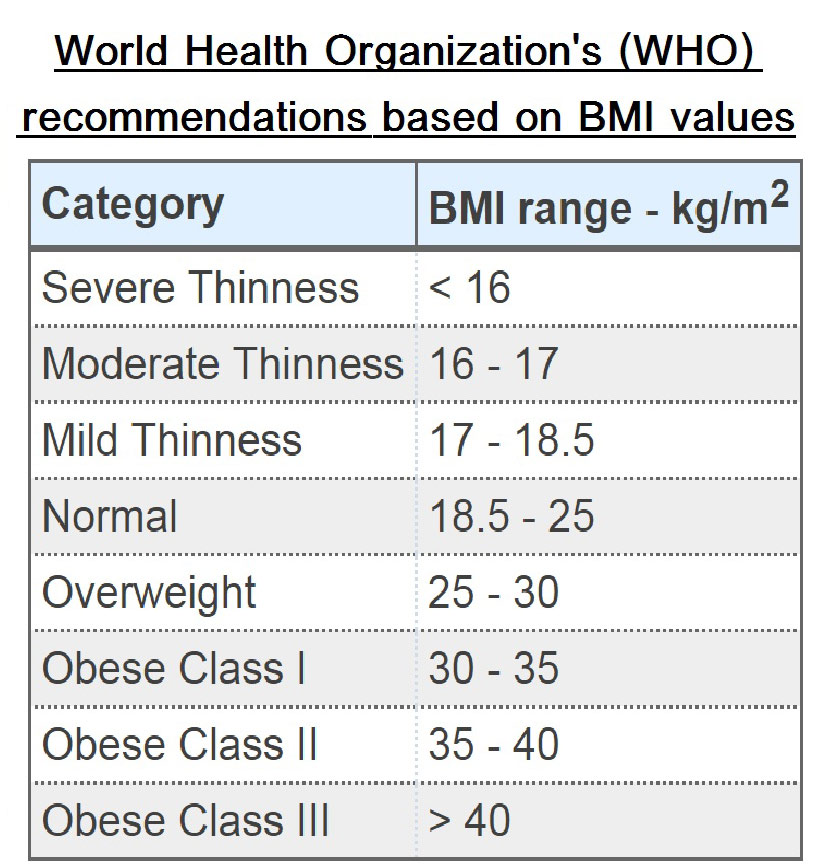
It might be argued that BMI does have one useful application in the clinical care of children: that is, it may be a more reliable indicator than visual inspection of progress made by a still-growing obese child whose weight control efforts are being monitored. However, for determining whether an individual child is obese, visual inspection-even from a distance of 30 yd-is superior to calculating his or her BMI. It is useful in population studies, providing a measure of “fatness” that can be easily plotted and compared. Body mass index (BMI) facilitates meaningful comparison of the weights of children of varying heights.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
